The most common symptom of IBS is abdominal pain. There are two main reasons that IBS causes pain. The first is because people with IBS are thought to have hypersensitive nerves in their gut, so even the slightest touch (such as from food passing through) can be very painful.
The other reason that IBS causes pain is because people with IBS have motility problems. Motility is the wave-like movements in the gut which propel food and waste through it. In IBS, the contractions can be very intense and chaotic, causing severe pain. You can read more about symptoms of IBS and what cause them here.
The first step in curing IBS is to understand exactly what is causing your symptoms. Different types of IBS pain have different causes. Here we will talk about the three main types of IBS pain and what is really behind them so you can get closer to finding a cure.
IBS Pain in the Lower Right Abdomen
More specifically, the pain is located about halfway between your bellybutton and your right hip bone. This is the area where your small intestine meets your large intestine (aka colon). Watery waste leaves the small intestines through a valve known as the ileocecal valve. This valve is very important because it prevents contents from your large intestine from backflowing into your small intestine. When your ileocecal valve is functioning normally, it will remain closed most of the time and only briefly open to let contents through.
If the ileocecal valve is not functioning normally, then contents of the large intestine will get into the small intestine. As one digestive specialist points out, this is a very bad thing because the two intestines have very different pH chemistry. The contents of the small intestine are meant to be absorbed, while the contents of the large intestine are meant to be eliminated. If juices from the two intestines mix, then gas will immediately be formed. This gas can cause pain as it pushes on the inside of the gut, and the pain can shift positions as it travels through the gut.
Why would your ileocecal valve malfunction? The reason is usually because the nerves controlling the ileocecal valve have become damaged. This leads us to the question of why the nerves would be damaged. The cause is usually an imbalance of bacteria in the gut, or irritation to the gut. We will talk about these underlying causes of IBS later in the series. (Source 1)
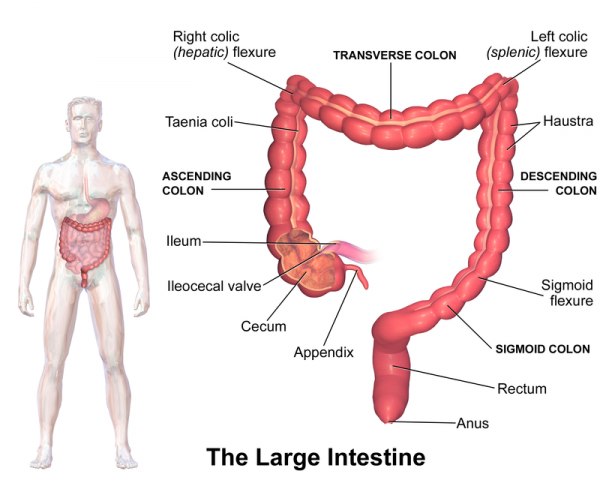
IBS Pain in the Upper Abdomen
The large intestine bends at two points located under the rib cage. These locations are called the hepatic flexure (right side) and the splenic flexure (left side). Because of the bent shape, pockets of gas can build up at these points. The pressure from the gas can cause severe pain. Some IBS patients even say that it feels like their ribs have been broken.
The pain can also occur in the unbent area between the two flexures (known as the transverse colon), especially when waste or gas gets backed up in this space. Pain in this area can confuse doctors because it might seem like liver, spleen, or even chest pain. (Source)
IBS Pain in the Left Abdomen
IBS pain most frequently occurs in the lower left abdomen. The pain can originate in the descending colon, which is the area of the large intestine where waste starts to become more solid. IBS patients often have hypersensitive nerves in their guts, so the solid waste can feel more painful than watery waste. (Source)
However, left abdomen IBS pain usually originates in an area called the sigmoid colon. The sigmoid colon is where feces are stored until it is ready to be expelled from the body, at which time they will be transferred to the anus and defecated.
The sigmoid colon is made up of several layers, including mucosa membranes (which produce mucus to help feces move through the colon) and smooth muscle tissue which contract to expel feces. The contractions of the sigmoid colon are more powerful than those in other areas as it needs to force fecal matter into the rectum. These contractions can be quite painful for people with IBS. (Source)
Studies have found that people with IBS have noticeable changes to their sigmoid colon, including:
- Increased thickness of sigmoid colon muscles
- Significantly greater, more frequent, and chaotic contractions of the sigmoid colon
- Higher pressures in sigmoid colon during contractions
- Increased electrical activity in sigmoid colon
The combination of spastic contractions and increased neural sensitivity can cause severe lower left abdominal pain for IBS patients. Note that the spastic contractions aren’t just limited to the sigmoid colon. These contractions can occur throughout the large intestine, causing pain anywhere in the abdomen. (Source)
Do you have IBS pain? Download our free guide 7 Things You Wish Your Doctor Told You About IBS and get closer to a cure.

Latest posts by Sylvie McCracken (see all)
- Treating H. Pylori (Part 3): What H. Pylori Does to the Body - August 8, 2022
- Treating H. Pylori (Part 2): How H. Pylori is Contracted - August 3, 2022
- Understanding Beef Labels: Organic, Pastured, Grass-Fed & Grain-Finished - July 25, 2022

Thanks for the clarification!
Could you please bring me up to speed on the subject of gelatin supplementation during SIBO healing? I am on Xifaxan currently and would like to take Great Lakes gelatin as a supplemental food to heal my gut during and after Xifaxan treatment. Gelatin supplementation doesn’t cause any SIBO symptoms for me. So is it safe to supplement?
I read in your book that bone broth made with knuckle/cartilaginous bones should be avoided. Some questions: 1. How long should cartilaginous bone broth be avoided? At what point can I reintroduce it? and 2. Is it ok to supplement gelatin during treatment and beyond even though it’s not ok to consume gelatinous broth?
Thank you for your help.
Thank you for this article. I recently bought your SIBO ebook and have a question. Regarding foods on the Yes/No list, when there are amounts specified (e.g., broccoli < 1/2 C), is this per meal or per day? Thank you!
Per meal Lucy. 🙂 Although of course you have to tailor it to you. If there’s a particular food that you can’t tolerate more than a couple times a week for instance you’ll have to restrict it differently. Hope that helps! Hang in there.
Sylvie